What is FHH?
Familial hypocalciuric hypercalcemia (FHH) is a very rare genetic condition that causes high blood calcium levels. It likely does not cause symptoms, and does not need to be treated. But be careful! Most of the time, high blood calcium is due to parathyroid disease, not FHH. The distinction matters, because the treatment is very different (do nothing for FHH, surgery for parathyroid disease). Most of the time, when we see someone who is diagnosed with FHH, he or she actually has a parathyroid tumor and needs an operation.FHH is very rare. If you have high calcium levels, the odds are that you have a parathyroid tumor, and not FHH.
FHH: What is FHH?
FHH is the abbreviation for a genetic medical condition called: Familial Hypocalciuric Hypercalcemia or: Familial Hypercalcemic Hypocalciuria
- Familial = occurs in multiple members of the same family (it is a genetic disease)
- Hypocalciuric = low amount of calcium in your urine
- Hypercalcemia = high amount of calcium in your blood
Thus, FHH is a very rare disease that runs in families which is associated with a higher than normal amount of calcium in the blood and a lower than normal amount of calcium in the urine. People with FHH have high calcium levels their entire lives - it is normal for them, and does not need to be treated.
FHH can also be called: Familial Benign Hypercalcemia.
FHH does not require treatment, and cannot be helped by parathyroid surgery.
If your doctor has never mentioned FHH, then you do not need to read this page. If your doctor said "Your urine calcium level is low so I think you have FHH, and you don't have primary hyperparathyroidism", then this page is for you. We see thousands of patients every year with high blood calcium, and we see a real case of FHH about once or twice year. If your calcium is high, and your PTH is above 35, the overwhelming odds are that you have a parathyroid tumor and your doctor is wrong - you do not have FHH. This is important because if you have a parathyroid tumor you need an operation to remove it; if you have FHH, then avoid surgeons - an operation will not help you.
What are the symptoms of FHH?
In general, FHH does not cause symptoms. People with FHH will always have high calcium levels, because their "normal" is high.
Why do we care about FHH?
The problem is that parathyroid disease can be mistaken for FHH. Most people with high calcium in the blood have a disease called primary hyperparathyroidism which is caused by a tumor of one of the parathyroid glands. We do not treat FHH, but primary hyperparathyroidism must be treated. Unlike FHH, parathyroid disease can be devastating if left untreated. See our page on the symptoms of hyperparathyroidism. It is very important to separate out those people who have hyperparathyroidism and need an operation to feel better and to preserve their health, from those with FHH who need no treatment.For those with primary hyperparathyroidism, removing the parathyroid tumor that is causing the disease will cure the disease (forever). You will feel better and live longer. For those with FHH, the high calcium is not caused by a parathyroid tumor so removing a parathyroid gland won't help.
Most patients who are told that they have FHH do not have FHH. They have primary hyperparathyroidism.
How Do We Diagnose FHH?
Because FHH is a genetic disease, the definitive way to diagnose it is with genetic testing discussed below). But some doctors try to diagnose it with urine calcium results. This is the logic used: FHH produces high blood calcium and low urine calcium. Parathyroid disease produces high blood calcium and often (but not always) high urine calcium. Thus, some doctors believe that anyone with a high blood calcium and a low urine calcium must have FHH.
What is low? Some doctors chose to use 100 mg/24 hours (less than 100 mg of calcium found in a urine sample collected over 24 hours) as an arbitrary cutoff for what is considered "low urine calcium." A doctor using urine calcium to diagnose FHH would claim that any 24-hour urine calcium result under 100 meant that the patient had FHH. But the problem is that low urine calcium can also be seen in primary hyperparathyroidism. And because primary hyperparathyroidism is so much more common than FHH, if you have a high blood calcium and a low urine calcium, the odds are that you have primary hyperparathyroidism - not FHH.
Low urine calcium cannot be used to diagnose FHH
Let's look at 10,000 patients that we operated on and removed a parathyroid tumor. Each dot on this graph represents a patient with high blood calcium. They all had primary hyperparathyroidism which is not in doubt because they had an operation where a parathyroid tumor was removed from their neck and after the operation they no longer had high blood calcium.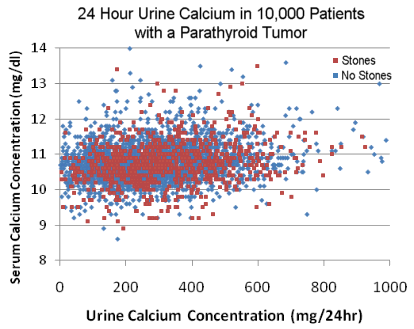
The vertical axis shows the blood calcium level, showing that the majority (but not all) patients with primary hyperparathyroidism have blood calcium levels above 10.1 mg/dl. The horizontal axis shows the amount of calcium in the urine of these 10,000 patients (always measured over a 24 hour period). The first thing that you will notice is that the 10,000 dots are completely random; they flow consistently from very low urine calcium levels to very high urine calcium levels. The second thing you see is that patients with parathyroid tumors can have very low urine calcium levels, medium (normal) urine calcium levels, or very high urine calcium levels. The third thing that you can see is that patients with parathyroid tumors who have very high blood calcium levels are NOT more prone to have high urine calcium levels (patients with higher blood calcium levels do not have a higher propensity to have high urine calcium levels). And finally, notice that we colored the dots red and blue, with red dots representing patients with primary hyperparathyroidism due to a parathyroid tumor in their neck who had calcium kidney stones, while the blue dots represent those patients with a parathyroid tumor but they do not have kidney stones. You can easily see that patients with parathyroid tumors can have kidney stones regardless of their blood calcium levels, and regardless of their urine calcium levels. Said differently, you cannot predict which patients with primary hyperparathyroidism will get kidney stones based upon how high their blood calcium levels are or how high their 24-hour urine calcium levels are.
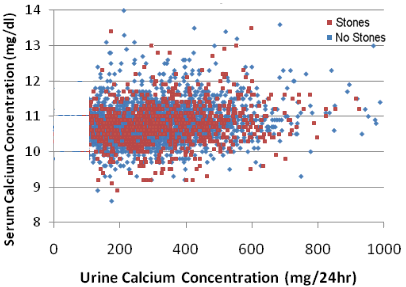
This is the same graph but we removed all the patients who had a 24-hour urine calcium level of less than 100 mg. If the decades-old teachings were right and the level of 100 was accurate in determining who had FHH and who had primary hyperparathyroidism then the graph would look like this. Of course this is absurd. The number 100 is simply arbitrary because it is a nice round number, but the real world is not this simple. The data clearly shows that patients with primary hyperparathyroidism don't naturally fall with a nice grouping above the number 100. They fall with a nice grouping from way down around 20 to way up to 1000 (as seen in the first graph). The problem is the arbitrary number of 100--it is simply dumb. So if your doctor told you that you have FHH because your 24-hour urine calcium is below 100, then he/she is wrong.
It is IMPOSSIBLE to tell the difference between FHH and primary hyperparathyroidism based upon the results of a 24-hour urine test.
NOTE: these graphs are included in the CalciumPro Parathyroid Diagnosis App. You can learn more about parathyroid problems and interact with the graphs on this page on your iPad or Android device. If you are reading this far on this page, then you may want to consider the CalciumPro app.
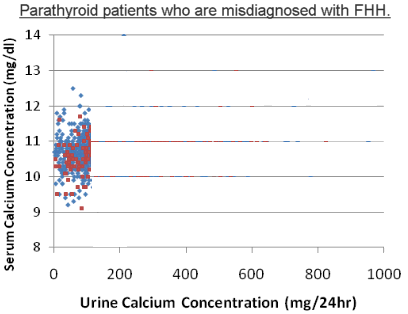
The third graph in this series shows 418 patients (out of 10,000 = 4.2%) that we have operated on for primary hyperparathyroidism and removed a parathyroid tumor. Some of them had doctors who knew they had a parathyroid problem even though their 24-hour urine was less than 100. Many of them were told that they had FHH and that they should not have a parathyroid operation because they did not have a parathyroid tumor - simply because their 24-hour urine calcium was less than 100. The patients either sought the advice of a different endocrinologist, or they (and their primary care doctor) figured it out for themselves and underwent surgery.
Another important point that is made clear by the third graph is that there are lots of patients here that have kidney stones. As you will recall from the blue symptom table at the top of this page, patients with FHH do not get kidney stones, but patients with primary hyperparathyroidism can get stones. You simply cannot differentiate between FHH and primary hyperparathyroidism based upon the amount of calcium in the urine.
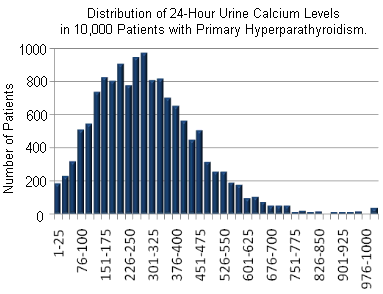
The next graph shows the 24-hour urine calcium results for the same 10,000 patients with primary hyperparathyroidism. This time we present the data in a bar graph so you can see how often patients with a parathyroid tumor actually have a 24-hour urine test with a result less than 100. It happens 4.2%, thus one out of 20 people with primary hyperparathyroidism will have a low 24-hour urine test, and if their doctor doesn't know better, he/she will tell the patient that they have FHH and they do not. Remember from above, this is very important because FHH is a "nothing" problem (you don't do anything about it because it causes no problems), whereas primary hyperparathyroidism causes lots of problems, lots of symptoms, and will slowly destroy a patient's body and overall health.
Genetic Testing for FHH
OK, so now we all understand that almost all people who have high blood calcium will have a parathyroid tumor in their neck and this high calcium is not normal for them. They have not had high calcium their entire life... they had normal calcium levels (typically in the mid 9's) their entire life until they grew a tumor on one of their parathyroid glands. The parathyroid tumor makes too much parathyroid hormone which in turn takes calcium out of the bones and puts it into the blood. The high blood calcium in these folks came from their bones! These people get symptoms, they get sick, they get bad osteoporosis, they get kidney stones, they get high blood pressure, they get all sorts of bad things happening because of the high calcium and PTH in their blood.
In contrast, a very small minority of people with high calcium in their blood (extremely rare) will have FHH. This means it is normal for them to have this slightly higher blood calcium. They don't get sick. They don't get osteoporosis or stones. They just have a higher "normal" calcium level in the blood.
So if FHH is a genetic disease, we should be able to use modern technology to examine a patient's DNA to find the bad gene that is responsible for this "higher normal" blood calcium level. And yes we can. There are several companies now that can do this test for you. Two things to remember, 1) it is not cheap, and 2) it is not always correct either! Most of the times the results will say "moderate probability of FHH", or "high probability of FHH". See, even these genetic tests are not always correct (because they have "control" DNA in their database that came from people with primary hyperparathyroidism but were misdiagnosed as FHH because of a urine calcium level below 100! How crazy is that?!). Even the companies that do the genetic testing will tell you that 10% of patients with FHH will not have a genetic defect.
FHH Technical Genetic Information
Familial hypocalciuric hypercalcemia (FHH) is an autosomal dominant condition caused by mutations in the calcium sensing receptor gene (CASR). FHH is characterized by hypercalcemia, hypocalciuria, hypermagnesemia, and normal to low levels of parathyroid hormone (PTH).
FHH is caused by loss-of-function mutations in the CASR gene. To date over 100 different alterations in the CASR gene have been described. Many of these cause diseases of abnormal serum calcium regulation. Inactivating mutations result in undersensing of Ca(++) concentrations and consequent PTH overproduction and secretion. This leads to either familial hypocalciuric hypercalcemia (FHH) or neonatal severe primary hyperparathyroidism (NSPHT), depending on the severity of the functional impairment. Homozygous or compound heterozygous loss-of-function mutations in CASR result in neonatal severe hyperparathyroidism (NSHPT) a severe and possibly lethal condition. Symptoms appear in infancy and include extreme hypercalcemia, failure to thrive, hypotonia, skeletal demineralization, and severe parathyroid hyperplasia. Some de novo mutations may cause a mild or transient version of NSHPT. Treatment may require parathyroidectomy in these very young infants.
Except for a very small percentage of cases with no apparent CASR mutations (maybe because they don't have the disease?), FHH is due to heterozygous inactivating CASR mutations. Serum calcium levels are mildly-to-moderately elevated. Parathyroid hormone (PTH) levels are within the normal range, phosphate is normal, and urinary calcium excretion is low for the degree of hypercalcemia. In contrast to patients with primary hyperparathyroidism, the majority of FHH patients do not seem to suffer any adverse long-term problems from their high blood calcium (hypercalcemia).
Calcium Clearance to Creatinine Clearance Ratios:
Patients with apparent mild-to-moderate hyperparathyroidism, who have a ratio of calcium clearance to creatinine clearance that is <0.01, could possibly have familial hypocalciuric hypercalcemia (FHH). Identification of a heterozygous inactivating CASR mutation confirms this diagnosis, while identification of novel alteration(s) increases the likelihood of a FHH diagnosis, but does not confirm it until family studies or functional studies support the diagnosis. Absence of any mutations or the presence of polymorphism(s) that are known to be functionally neutral makes the diagnosis very unlikely.
Approximately 20% of FHH patients are reported to have calcium to creatinine clearance ratios of >0.01. These patients can be difficult or impossible to distinguish from individuals with primary hyperparathyroidism (PTH).
FHH vs Primary Hyperparathyroidism: The Bottom Line
Bottom line is this: If your blood calcium is high, the odds are that you have a parathyroid tumor that is causing primary hyperparathyroidism. Genetic testing is used to diagnose FHH - urine calcium should never be used for diagnosis. Most of the time, if you have FHH, then other members of your family will have it as well.
Remember, many people diagnosed with FHH do not have FHH. If your doctor says you have FHH based only upon your urine calcium level, then demand a genetic test. The diagnosis of FHH should never be made without a genetic test. And then, know that most genetic tests for FHH will be equivocal and they will not come out and say yes/no.
This page was last updated: 11/01/2021




