How do you diagnose Hyperparathyroidism / parathyroid disease?
Hyperparathyroidism is diagnosed by measuring the amount of calcium and parathyroid hormone (PTH) produced by parathyroid glands in the blood. If both are high, the diagnosis of hyperparathyroidism is made. In 20% of patients, the calcium is high and the PTH is normal. A high PTH level is not required to diagnose this disease.
This is an advanced page aimed at helping doctors (and knowledgeable patients) make the swift and correct diagnosis of primary hyperparathyroidism. This and the video page are two of the best pages of this website. The information here is based upon our experience with over 35,000 patients that we have operated on for parathyroid disease. We use a lot of graphs in a combined fashion to build a logical method for the correct, swift, (and cheap) diagnosis of primary hyperparathyroidism. All of these graphs and more can be found on our CalciumPro app for smart-phones and tablets. If you are on this page, then you should get the app so you can put your data on all of these cool graphs.
Let's start with normal and abnormal calcium levels. The illustration below shows that the normal range for calcium as reported with a patient's labs is between 8.6 and 10.2 mg/dl (some go as high as 10.4). However, almost all adults actually live in the 9's. It is uncommon for an adult over age 40 to have persistent calcium levels above 10.1 or below 9.2. It is OK to have a calcium level in the 10's on occasion (infrequently), but usually when checked again it will be back in the 9's. Calcium levels that are consistently in the low to mid 10's (in an adult over 40) are usually caused by a parathyroid tumor. Remember this rule: Most adults over age 40 will live in the 9's, not the 10's. An occasional calcium level in the low 10's is ok.
Start at the top left of this illustration and work your way around clockwise to examine what normal calcium levels are and what it means to have a high calcium level.
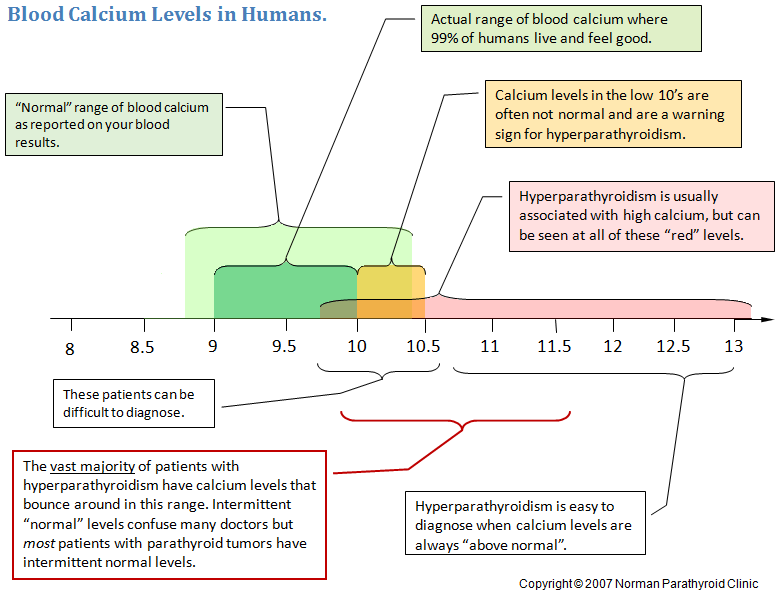
It is classically taught that the diagnosis of hyperparathyroidism requires a high calcium and a high PTH level at the same time. Unfortunately, about 20% of patients will not follow this pattern, with some having high calcium levels and all normal PTH levels (18%), while others have normal calcium levels with high PTH levels (2%). This will be looked into extensively below. A high calcium and a high PTH at the same time is absolutely NOT required to diagnose primary hyperparathyroidism!
The First Step in Building our Calcium/Parathyroid Hormone Normogram.
The following graph shows normal calcium levels (between 8.8 and 10.2 mg/dl) on the X-axis which are then graphed according to normal parathyroid hormone (PTH) levels (between 14 and 65 pg/ml) on the Y-axis. This produces a green box where all of us healthy humans live. Remember, calcium is the means by which our nerves conduct impulses and by which our muscles contract. Our brains and muscles don't feel good outside this box. Our calcium is maintained in the green box by the actions of our parathyroid glands making the appropriate amount of PTH. We will build on this graph multiple times as this page progresses.
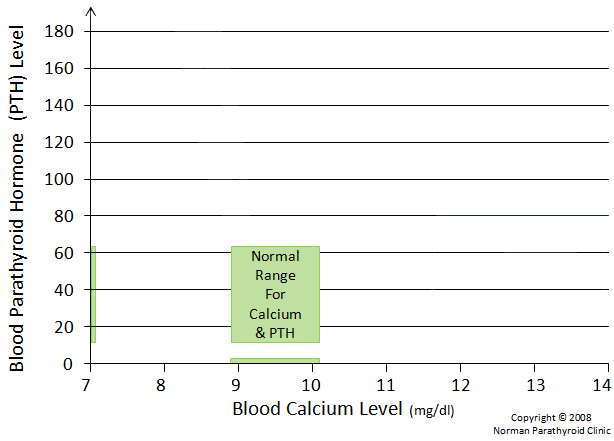
What are Calcium Levels in Primary Hyperparathyroidism?
98% of patients with primary hyperparathyroidism have high blood calcium, above 10.0 mg/dl in adults over 40 years of age, and above 10.5 for young people. High blood calcium is almost always caused by hyperparathyroidism. Two percent with primary hyperparathyroidism will have normal calcium levels.
The following graph looks at blood calcium levels in 30,000 patients with symptomatic hyperparathyroidism from whom we removed a parathyroid tumor. Note that the average calcium level for somebody with primary hyperparathyroidism is 10.8, with a mode of 10.7, and a standard deviation of 0.591. Importantly, 85.6% of patients with a parathyroid tumor and symptomatic hyperparathyroidism have an average calcium level of 11.5 or lower, with 68% of them never having a single calcium higher than 11.4.
Blood calcium level normogram for the diagnosis of primary hyperparathyroidism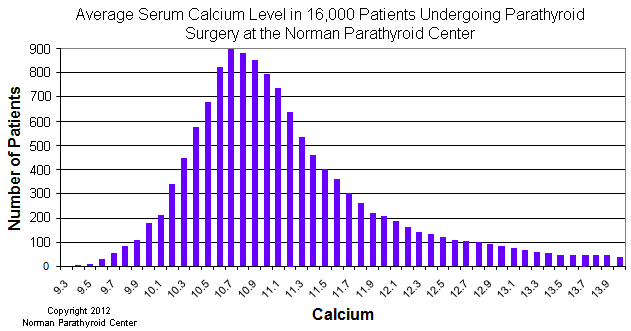
A common mistake we see occurs when a doctor will make a recommendation to a patient with high calcium to "watch and wait" to see if the calcium goes above 11.5. The thought process is that below this number it's ok to have high calcium, but above this "magic" number something should be done. It is absolutely unclear where this "magic" number came from (we know it is propagated in the NIH consensus guidelines), but there has never been a single study to suggest this "magic" number, and there is no scientific basis for this. Two thirds (68%) of patients with a parathyroid tumor in their neck making them sick will never achieve a calcium level this high regardless of any other issues (stones, osteoporosis, etc, etc). Calcium levels are an independent parameter and as such, it is impossible to predict which patients will develop higher calcium levels and which will be stuck below 11.5 until they quit your practice to find another doctor that will help them. As is discussed in great detail on another page of Parathyroid.com, the severity of symptoms or the number of symptoms a patient has is absolutely unrelated to the degree to which their calcium is elevated... with one exception: severe symptoms such as stroke increase in frequency with increasing calcium levels. Note just how few patients there are on the graph above that have calcium levels of 12 or higher. If you are waiting until your patient has a calcium level of 11.5 to send them to a surgeon, this is not proper. It will probably never happen and they will continue to suffer.
The second important aspect of the purple bar graph above is to note how many patients have "normocalcemic" hyperparathyroidism. That is, their calcium levels are normal yet they have symptoms of hyperparathyroidism that were cured by removing a parathyroid tumor. Approximately 2% of all patients with hyperparathyroidism will have average calcium levels that are in the normal range. "Normocalcemic hyperparathyroidism" is discussed in more detail below, but this can be a tough group to diagnose.
What are Parathyroid Hormone Levels in Patients with Primary Hyperparathyroidism?
Parathyroid hormone (PTH) levels can be either normal or high in patients with primary hyperparathyroidism. Most will have high PTH levels, but 18% will have normal PTH levels.
The following graph shows average parathyroid hormone (PTH) levels in 18,000 patients in whom we removed a parathyroid tumor for primary hyperparathyroidism. Note how many of these patients have average PTH levels in the "normal" range (below 65 pg/ml)... 2986 out of 18,000. Of course all of these patients had high calcium levels making their "normal" PTH levels what we call "inappropriately normal" parathyroid hormone secretion. Editors Note: We examined this data again in December 2022 and looked at our last 40,000 patients who had a parathyroid tumor removed, and 8.5% never had a single elevated PTH level. You don't need a high PTH level to make the diagnosis of primary hyperparathyroidism (but it can't be low normal or low).
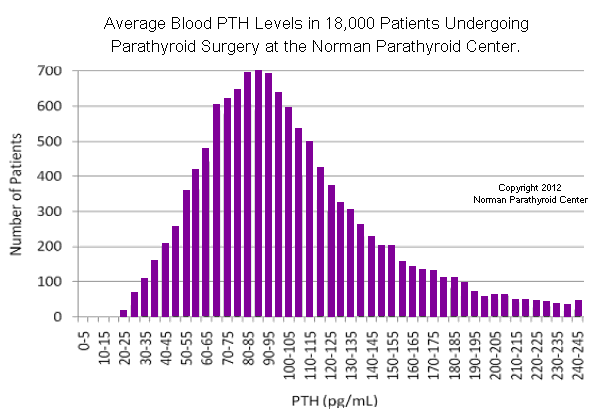
It is absolutely not necessary to have high PTH levels to make the diagnosis of hyperparathyroidism... but if the PTH is not high, then the calcium must be high (and the PTH levels are usually over 35 pg/ml). This is examined later in more detail. Thus, most of the time, calcium and PTH are both high, about 18% of the time the calcium is high and the PTH is normal, and about 2% of the time, the calcium is normal and the PTH is high. (This later group can be difficult to diagnose but almost always the PTH levels are above 105 pg/ml).
Building the Primary Hyperparathyroidism Normogram:
Adding PTH Levels Onto our Normal Calcium Box
On this graph we've superimposed the PTH data onto our graph with the green box. Virtually 100% of all patients with primary hyperparathyroidism can be plotted onto this graph within the blue area. As we can see, some can have normal calcium with high PTH (top left part of the blue area), some can have high calcium with normal PTH (bottom part of the blue area). But most will have high calcium and high PTH.
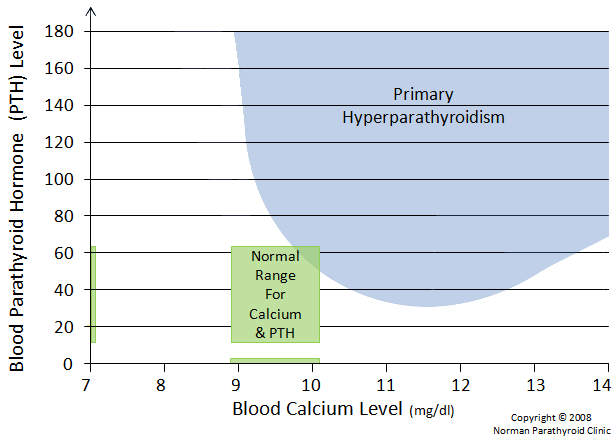
"Confusion Areas" A & B, Defining the Easy to Diagnose and Hard to Diagnose
Now we will look at the blue area closer. We have superimposed two more darker blue areas which represent the vast majority of patients with primary hyperparathyroidism. The large oval represents 80% of all patients with primary hyperparathyroidism. The smaller blue oval represents 50% of all patients with primary hyperparathyroidism. So even though the overall blue area is quite large and includes patients with dramatically different biochemical profiles, the vast majority of patients have classic high calcium and high PTH. These patients should be quickly diagnosed and sent for tumor removal.
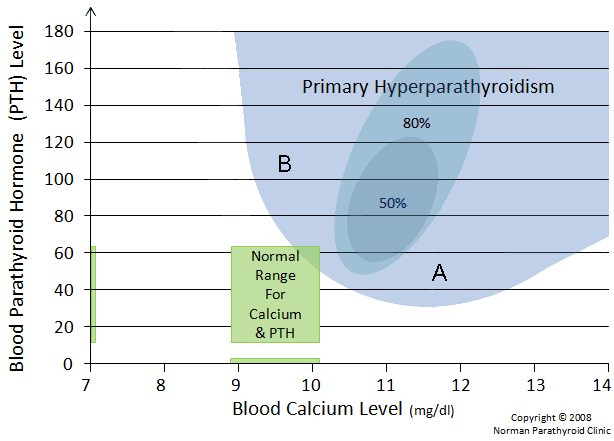
Note that we've added "Confusion Area A", and "Confusion Area B". Patients who fall into one of these two areas on our graph are frequently misdiagnosed by even the most respected endocrinologists (they don't see enough patients in these two areas to have much experience). Patients in "Confusion Area A" are those with high calcium levels with normal PTH levels. We operate on somebody in this category every day, so it is quite common. But, these patients are often misdiagnosed for many years as the well-meaning doctor checks and re-checks their blood... hoping that the PTH will some day be above normal so they can make the diagnosis of primary hyperparathyroidism with confidence. This is most unfortunate. Hopefully after reading this page you will understand that high calcium levels means primary hyperparathyroidism unless the PTH is very low (under 20).
Patients in "Confusion Area B" have "normocalcemic" hyperparathyroidism. That is, they have hyperparathyroidism due to a tumor in the neck just like all other patients with primary hyperparathyroidism, but their blood calcium levels are normal. These patients typically will have a high ionized calcium level in their blood, and may have a high urine calcium level. The diagnosis is made clear when many other clinical data are examined. These patients are the hardest patients to diagnose, and we usually need to evaluate many lab values over time, including total calcium, ionized calcium, PTH, and Vitamin D levels.
Finally, there are a few RARE patients who are in the white area BELOW the Confusion Area A... Ionized calcium levels may be useful in all of these confusing patients. There are some very rare patients outside of the blue area, but they are very difficult to diagnose. Many other clinical issues need to be examined (bone density, urine calcium, variability of the labs, etc).
High Calcium Associated With Malignancy.
Easy to Differentiate from Primary Hyperparathyroidism.
Let's look at patients with high calcium in their blood due to advanced cancer and see where these patients fit on our calcium normogram.
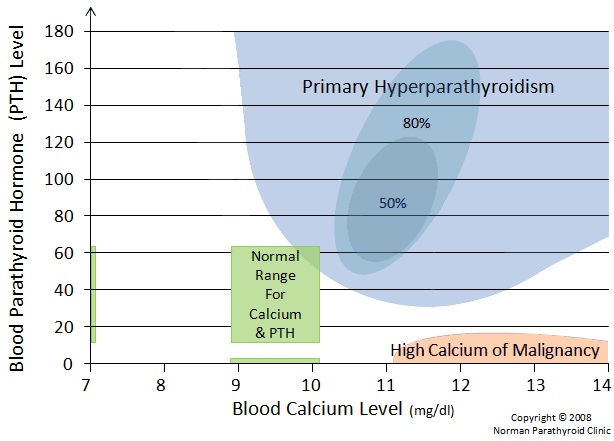
Usually, patients with hypercalcemia due to cancer are sick and dying of their cancer. It isn't a surprise to anybody that they have cancer... it's advanced cancer. When the calcium is high due to cancer, the normal parathyroid glands will shut down in the face of high calcium levels. Thus, normal parathyroid glands will make very little hormone in the presence of high blood calcium. High calcium levels due to cancer will virtually always be associated with PTH levels below 20, often below 10.
Vitamin D Deficiency and its Relationship to Primary Hyperparathyroidism.
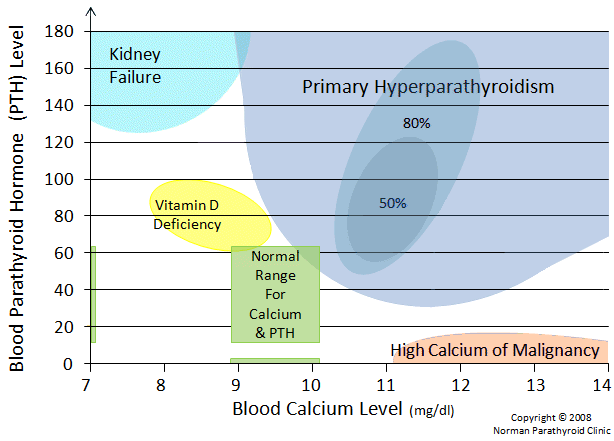
This graph shows where patients with a vitamin D deficiency fall onto our calcium normogram. Low Vitamin D levels can lead to low calcium, which in turn raises the PTH level.
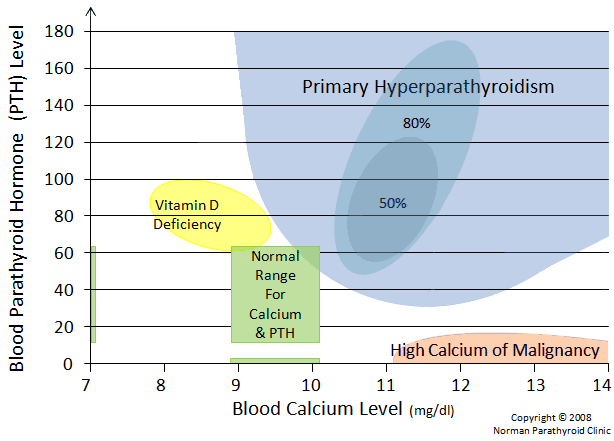
It has been suggested (wrongfully) that low Vitamin D levels will cause normal parathyroid glands to hypertrophy and over-produce PTH... which in turn will cause the calcium to rise. This does not happen. Low Vitamin D levels will NEVER cause the calcium to increase above normal. Low Vitamin D does not ever cause a high calcium. It is possible, as shown on the graph above, that low vitamin D levels in patients with low-normal or low calcium levels will be associated with modest elevations in the PTH. But that's as far as it goes. Low Vitamin D will not produce a cascade of events that lead to high calcium levels in the blood. Remember, most patients with tumor-proven primary hyperparathyroidism will have LOW Vitamin D levels.
Read more about Vitamin D in primary hyperparathyroidism on this page. It describes in more detail that the low vitamin D-25 is caused by an increased conversion to 1-25 Vitamin D... the 1-25 vitamin D is high, and the active form (Vit-D25) is LOW. Read more on our Vitamin D page.Secondary Hyperparathyroidism Due to Kidney Disease.
The next set of patients that cause confusion in the diagnosis of PRIMARY hyperparathyroidism are those with renal insufficiency (kidney failure). All patients with severe kidney failure on dialysis will develop SECONDARY hyperparathyroidism to some degree or another. All four of their parathyroid glands become enlarged and overproduce parathyroid hormone (PTH) in response to the high phosphorus in the blood associated with renal failure. Thus, their parathyroid glands become enlarged "secondarily" to (caused by) the kidney disease. These patients generally have normal or low normal calcium levels and VERY high PTH levels (250 to 4000--way off the top of our graph). These patients do not have a single parathyroid tumor... they have four big juicy glands that are responding appropriately to the high serum phosphorus and are trying to signal the kidney to do the right thing. Unfortunately the kidney has failed and cannot respond, and the parathyroid glands just keep trying harder.
We see confusion between primary hyperparathyroidism and secondary hyperparathyroidism due to kidney disease on a daily basis...however, this really shouldn't be confusing! The confusion arises when a patient with primary hyperparathyroidism (high calcium, high PTH) will be noted to have a high creatinine and/or BUN in their blood. These are measures of kidney function and when elevated usually indicate that the kidney has lost some of it's function. HOWEVER, secondary hyperparathyroidism will almost never occur in patients unless they have such severe kidney function that they are on dialysis, or at least had significant kidney problems for many years (it isn't a secret that they have kidney problems). Patients with high calcium, high PTH, and modest elevations in their creatinine and modest or even significant decreases in their GFR (glomerular filtration rate)... have PRIMARY hyperparathyroidism and need an operation to remove their ONE parathyroid tumor. In fact, it is VERY LIKELY that the long-standing PRIMARY hyperparathyroidism is causing the kidney failure! Please understand this paragraph, as we see people misdiagnosed in this category every single day! Secondary hyperparathyroidism occurs in patients with SEVERE renal function for YEARS... it is not subtle, and it is NOT associated with high calcium levels! High calcium levels with high PTH levels in a patient with modest increases in creatinine and BUN have PRIMARY hyperparathyroidism... they need an operation urgently to remove their one parathyroid adenoma to prevent further kidney destruction.
High Parathyroid Hormone Levels in Patients with Intestinal Absorption Problems, Such as Gastric Bypass Surgery, Celiac Sprue, and Crohn's Disease.
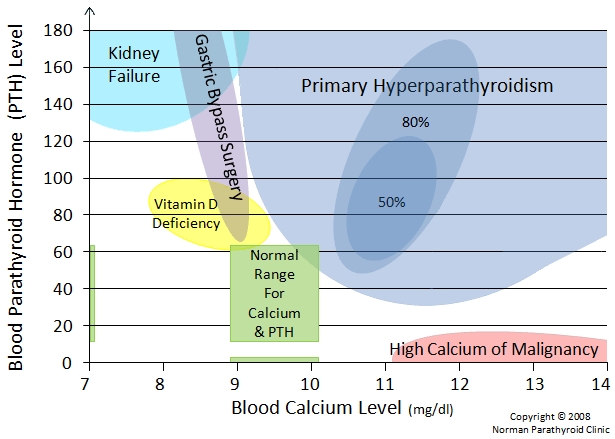
There is a growing group of patients who have dramatic life-long problems absorbing calcium in their diet. These patients are illustrated on our graph in the purple area. These patients have difficulty absorbing calcium from their intestines, and end up with chronically low blood calcium levels as a result. Since they don't (can't) absorb calcium from their diet, their NORMAL parathyroid glands will do what they are supposed to do in order to try to maintain a proper calcium level in the blood. There is only one thing these normal parathyroid glands can do... all four glands enlarge and produce lots of PTH which removes calcium from the bones--it's the only place to get the calcium. The blood calcium will usually be in the low-normal range between 8.2 and 9.2 mg/dl, but can be as low as 7.0. Thus these patients can develop very significant osteoporosis, high PTH levels, and high alkaline-phosphatase (shows increased bone destruction). These patients have developed a total-body calcium deficit due to a longstanding inability to absorb calcium through their intestines. This is a form of secondary hyperparathyroidism, and should be treated with calcium and Vitamin D supplementation.
The most common people in this purple group are 1) those who have had gastric bypass surgery for weight loss, 2) those with chronic diarrhea, most commonly from Celiac or Crohn's disease, and 3) those who have had a significant part of their intestines surgically removed. Most of the calcium that gets absorbed in your intestines is absorbed in the duodenum, the first part of the small intestine. During a gastric bypass, the duodenum is bypassed, so the food does not encounter the area where most calcium absorption should occur, which leads to chronic malabsorption of calcium. This will happen to all patients who have had a gastric bypass or gastrectomy with Roux-en-Y reconstruction. The treatment is lifelong calcium and Vitamin D supplementation to help the intestines absorb enough calcium. Most people with secondary hyperparathyroidism due to a gastric bypass do not need parathyroid surgery. They need more calcium and Vitamin D. In most cases, bringing the calcium level up will lead to a reduction in the PTH levels.
Chronic diarrhea due to celiac or Crohn's disease will also lead to an inability to fully absorb calcium, which leads to a total-body calcium deficit and secondary hyperparathyroidism. The best way to prevent this is to treat the underlying condition, the diarrhea. In Crohn's disease, many patients also need to have portions of their small intestines removed, which increases the difficulty in absorbing enough calcium.
Note that in all of the cases in which the PTH is high due to calcium absorption issues, the blood calcium level is LOW. If the calcium level is HIGH, then the cause of the PTH elevation is NOT malabsorption. It is a parathyroid tumor. Surgery is usually not necessary in cases of secondary hyperparathyroidism due to malabsorption. The treatment is increased supplementation with calcium and Vitamin D. If the calcium is HIGH, then it is primary hyperparathyroidism due to a parathyroid tumor, and surgery is the only treatment. Patients who have had gastric bypasses (or have Crohn's disease, or celiac disease, or chronic diarrhea due to any cause) can still get parathyroid tumors! If the calcium level is HIGH, then malabsorption is not causing the high PTH. A high calcium with a non-suppressed PTH in any patient - gastric bypass or not - indicates a parathyroid tumor.
Completed Picture of Updated Calcium/Parathyroid Hormone Normogram.
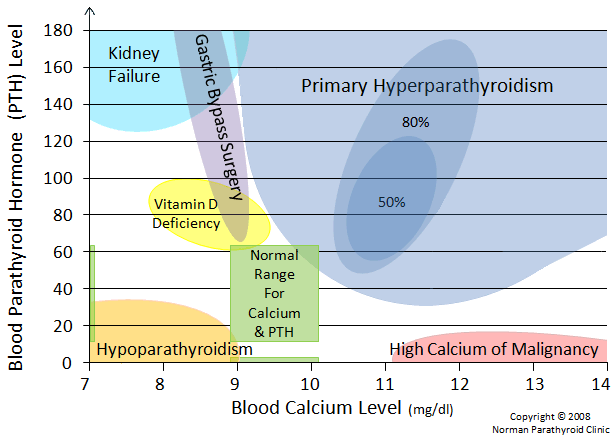
This is the completed Calcium Normogram, based upon our experience with many thousands of patients. Our graph of normal and abnormal calcium and parathyroid hormone is complete only after we add those patients with hypOparathyroidism. HypOparathyroidism is a disease of low parathyroid hormone secretion. This is covered on two separate pages of this website so it is not covered here. There should never be an instance where hyperparathyroidism and hypOparathyroidism are confused.
Low Vitamin D
The graph below is different from all the graphs above. The horizontal (X) axis is the same, but the vertical (Y) axis has been changed to show Vitamin D-25 levels. Again, the green box in the middle represents normal calcium levels for an adult, and normal vitamin D-25 levels (between 30 and 65 ng/ml). There are many people out there running around with low vitamin D, however, some of these people have low vitamin D for a non-dangerous reason, and some have low vitamin D because a serious problem exists. Let's talk about the non-dangerous (most routine) reason first: These people are represented by the yellow blob on this graph. These folks have low vitamin D because they are not getting enough in their diet, and/or because they don't go out in the sun enough (we make vitamin D in our skin when exposed to sunlight). These people simply need to be given some vitamin D (orally) so that they can continue to maintain good, normal blood and bone calcium. No big deal, if you have normal blood calcium and your vitamin D is low, then take vitamin D. It's not rocket science.
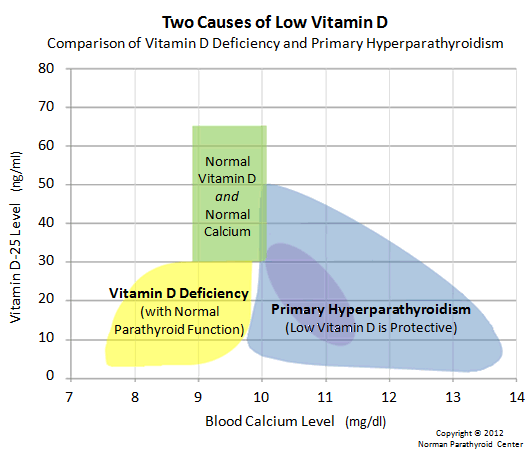
HOWEVER, there is a BAD reason for having a low vitamin D, and this is a sign that something else is wrong with the calcium in our bodies. The blue blob represents people with primary hyperparathyroidism (who need an operation to remove a parathyroid tumor from their neck). These people have high blood calcium (frequently or persistently above 10.1 mg/dl) because they have a parathyroid tumor in their neck. 84% of patients with primary hyperparathyroidism have low vitamin D-25. Note that this is compensatory and protective: the body has enough calcium and so it turns off vitamin D production--it simply does not want more calcium. Thus, the calcium is too high, we stop making vitamin D so we don't absorb more calcium in our diet. The purple area shows where 80% of patients with primary hyperparathyroidism are on this graph: 80% of patients with a parathyroid tumor have calcium levels between 10.2 and 11.4, and vitamin D levels between 8.5 and 31.5.
Remember, a LOW vitamin D cannot ever be the cause of a HIGH blood calcium level. This form of "secondary" hyperparathyroidism does not exist. There is no such thing as a low vitamin D causing hyperparathyroidism leading to high blood calcium. If your doctor says this, then you have some teaching to do. A patient with high blood calcium has a low vitamin D to protect them--do not give this patient vitamin D--they can develop severe high blood calcium levels and have a stroke. We've seen it! We have an entire page of this website dedicated to this graph (and a few others). If you are dealing with a "Low Vitamin D" problem, then it is time for you to go to our Low Vitamin D page and learn more about this graph and the role of vitamin D in maintaining good calcium health. If your vitamin D is low, then you need to know what your calcium is. If your vitamin D is low and your calcium is normal, then you need more vitamin D. If your vitamin D is low and your calcium is high (even a little high), then you do not want to take vitamin D, you want to take a trip to the operating room to get the tumor removed from your neck. Still want to know more about low vitamin D??? Go to our page on this topic.
Urine Calcium Levels. A Test that is Frequently Done, and RARELY Helpful.
Urine calcium levels are a tool that can occasionally be used to help make the diagnosis of hyperparathyroidism but usually just wastes time and makes people put their urine in their refrigerator for no good reason. This test is often obtained on patients with high blood calcium levels by physicians to "rule out FHH". But FHH is rare, and urine calcium testing can't rule it out anyway! Most of our patients who have been told they have FHH actually have hyperparathyroidism, and we prove the doctor wrong by taking a large tumor out of the patient's neck. (We have an entire page on FHH). FHH is a genetic disorder that has been written about more often than there are patients afflicted. A LOW calcium level in the urine associated with high PTH and high blood calcium means the patient has primary hyperparathyroidism. Period. FHH will not cause high blood calcium and high PTH! A doctor who is looking for FHH will frequently miss patients who have primary hyperparathyroidism but who reside in "Confusion Area A" on our graph. We have never seen a case where low urine calcium levels made us decide not to operate on a patient. We operate on patients every single day who have low urine calcium levels... and they all have a parathyroid tumor... of course, their labs fall into the blue area of the curve, and their clinical history and other data support the diagnosis. The graph here shows Urine Calcium levels (mg/24 hours) on the X-axis compared to Serum Calcium Levels (mg/dl) on the Y-axis in 10,000 patients with primary hyperparathyroidism. All of these 10,000 patients had a parathyroid tumor removed from their neck, thus the diagnosis of primary hyperparathyroidism is not in question.
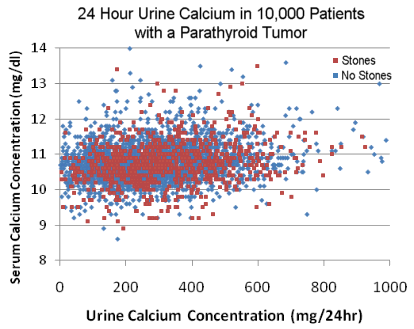
As you can see, there is no correlation between blood calcium and urine calcium in patients with hyperparathyroidism. That is, a patient with a blood calcium of 10.7 is just as likely to have a urine calcium level of 150 as he is to have a urine calcium level of 400. In fact, 44% of patients with a parathyroid tumor in their neck have a urine calcium level of 250 or below (normal levels). 11% will have urine calcium levels below 100, yet they still have primary hyperparathyroidism and they do NOT have FHH. Thus, measuring urine calcium on a patient with high blood calcium will simply put them somewhere on this graph... HOWEVER, it does not matter where they are on this graph since EVERYBODY on this graph has primary hyperparathyroidism and needs an operation to remove their parathyroid tumor.
As a final clarification about FHH, please note that there is no artificial cutoff at 100 mg/24 hours on this graph. To arbitrarily say that patients with urine calcium levels below 100 mg/24 have FHH and those above 100 have primary hyperparathyroidism is ridiculous. There is no such artificial cutoff--the data is a perfect scatter and patients with parathyroid tumors often have urine calcium levels that are low. Hey endocrinologist! Are you listening? You cannot make the diagnosis of FHH by measuring the amount of calcium in your patient's urine despite what you were taught.
We have a complete page on FHH which breaks down these 24-hour urine graphs even further. Again, the page on FHH is an advanced page and the only people who should read it are doctors and patients who were told they had FHH by a doctor. They almost certainly do not.
Another important point made very clear from this data is that (contrary to popular belief), the amount of calcium in the urine in a patient with primary hyperparathyroidism does NOT correlate with the incidence of kidney stone formation. As shown in this graph, patients who had stones (shown in red) have the exact same distribution of 24-hour urine calcium concentrations as those patients who did not have stones (shown in blue). Thus using the 24-hour urine calcium concentration as an indicator for surgical referral (as suggested in the NIH consensus panel guidelines) is without scientific basis. They "guessed" at an arbitrary number (400 mg/24 hours) as a level that "is likely" to result in a higher incidence of stone formation. They guessed wrong--there is no correlation and you cannot predict which patient with primary hyperparathyroidism will develop kidney stones by measuring the amount of calcium in their urine. The graph is a perfect scatter, with zero correlation (p=0.98). Stones do NOT form more frequently in parathyroid patients with high urine calcium than they do in parathyroid patients with normal or low urine calcium. You cannot predict who will get stones, who has a big vs. a small parathyroid tumor, who has one tumor vs. two tumors... based upon urine calcium levels. Urine calcium levels carry no predictive value and have nearly zero diagnostic value.
Our recent examination of the medical records of 1122 endocrinologists who referred us nearly 7000 patients between 2005 and 2010 shows that only 34% of them ever obtained a 24-hour urine test on a patient they were testing for primary hyperparathyroidism. When we consult with a patient regarding the potential diagnosis of primary hyperparathyroidism, we couldn't care less if they had a urine calcium level, unless they have normal serum calcium levels. If the blood calcium is high, then we don't care what the urine calcium is... it is often high, it is often normal, and it is often low (as seen on our graph). This test provides no useful information and carries no predictive value if the blood calcium is high. It is a worthless test in 95% of patients. Obviously, 66% of endocrinologists already have figured this out on their own.
Note, we use the terms blood and serum interchangeably on this page for the benefit of patients who are reading it. Of course we understand that we don't actually measure blood calcium levels, rather we measure the calcium concentration in the blood after the red blood cells have been removed, and thus the correct term would be serum calcium levels. But, everybody knows what we are talking about if we say blood calcium.
Sestamibi Scans and Ultrasound Scans.
Scans are mentioned here in the diagnosis section of parathyroid.com only to be condemned. Sestamibi scans are not diagnostic scans! We will say this again... sestamibi scans are not to be used to determine if a patient does or does not have hyperparathyroidism! Geeze, we even see doctors use this scan to tell the difference between primary and secondary hyperparathyroidism. Can you hear us jamming toothpicks into our corneas? If you use this scan for this purpose, you will make the wrong diagnosis almost half of the time! Flip a coin, it will be cheaper and faster. Sestamibi scans are not to be used to determine who has parathyroid disease, who doesn't, what kind of parathyroid disease they have, or who should have surgery or not. This scan CANNOT tell you this kind of information.
We review 4,200 sestamibi scans per year and have developed a grading system that examines the technical quality of the scan, and therefore, its worth. Nearly 80% of the scans we are sent for review are essentially worthless for the evaluation of parathyroid tumors. Unfortunately, many endocrinologists will obtain a Sestamibi Scan on a patient with obvious hyperparathyroidism because they feel better about the diagnosis and sending the patient for surgery when a tumor can be seen on an x-ray. We feel using a sestamibi scan for diagnostic purposes is the BIGGEST MISTAKE of all mistakes made in the diagnosis and treatment of primary hyperparathyroidism. These scans are not intended to be diagnostic scans. We have a paper out shortly showing that endocrinologist-obtained sestamibi scans delay surgery by 2.5 years when the scan is negative... even though the patient has obvious hyperparathyroidism by all laboratory studies. ALL SCANS (sestamibi and Ultrasound) are NOT diagnostic tests and should never be used to determine if a patient does or does not have hyperparathyroidism. Furthermore, the results of these scans should NEVER be used to make management decisions regarding who does or does not need an operation to have the tumor removed. In other words, deciding to send one patient for surgery because a scan is positive and telling another to "wait and see" because a scan is negative is not based upon any medical facts or clinical data. These patients are identical, their risk of osteoporosis is identical, their risk of kidney stones and renal failure is identical, their risk of stroke is identical, their increased risk for developing breast or colon cancer is identical, their risk of depression is identical, their symptoms of fatigue and irritability is identical, their risk of cardiac arrhythmias and heart attack is identical. A patient either has hyperparathyroidism or they do not. The results of a sestamibi scan or ultrasound should never have a role in the diagnosis aspect of primary hyperparathyroidism, or in determination of who is or is not a candidate for surgery.
Do we use sestamibi scans? Yep, absolutely... 100% of our patients get a scan... about 1 hour prior to their operation. We never obtain scans to determine who does or does not have parathyroid disease. We developed many of the techniques for a modern high-resolution sestamibi scan and its results are invaluable in the operating room. Most importantly, the injected isotope is what we use in the operating room to measure the amount of hormone produced in each individual parathyroid gland (in 2 seconds). The scan should play no role in the decision to operate; it is usually negative because of the poor technique used, and will need to be repeated immediately prior to the operation. Please do NOT get a sestamibi scan or ultrasound scan on your patient if they are going to come to us for surgery. We are running out of toothpicks!
Parathyroid Cancer
You may note that parathyroid cancer is not on our normogram... for good reason. For all practical purposes, it doesn't exist and is WAY over-reported by well meaning but inexperienced surgeons who find old, scarred tumors. Virtually 100% of the parathyroid cancer cases that are sent to us we change the diagnosis to benign parathyroid disease in an old, scarred tumor. That's it; we will no longer discuss diagnosing something that nobody will ever see. If you must read about it, it's covered on another page of this website that almost nobody should read.
Summary: The Diagnosis of Primary Hyperparathyroidism.
In summary, the diagnosis of primary hyperparathyroidism is made by looking at a patient's clinical presentation and their labs. NOT their x-rays. Most have a chief complaint of fatigue, but many other symptoms will be present in the vast majority of patients. As long as you understand that patients can have primary hyperparathyroidism with normal calcium levels or normal PTH levels, you will be able to make the diagnosis in almost every case. Remember, it is almost never normal to have high calcium levels, and this should typically be worked up with the presumption that a parathyroid tumor is present. Also remember that calcium AND PTH levels in normal patients are very constant from week to week, measure to measure... while those with primary hyperparathyroidism have calcium and PTH levels that go up and down from day to day, week to week. They are variable. There is no medical reason to "wait 6 months and get more tests". The patient either has a parathyroid tumor or they do not. The key to making the diagnosis of primary hyperparathyroidism is REPEATED measures of 1) serum calcium, 2) ionized calcium, 3) PTH. Measure them weekly for 2 or 3 weeks and the diagnosis will be clear in almost all cases. Adults over 30 live in the 9's, not the 10's. Teens and young adults in their 20's who are building bone can have calcium levels up to 10.7 on more than one occasion. Generally, this is not true for adults over 30. There is no reason to wait any more than 1 week for repeat lab tests, and there is no reason to get a urine calcium level on the vast majority of patients--its a test with no value. Finally, remember that getting scans is NOT part of the diagnosis of hyperparathyroidism.
We published this information:View a PDF of our publication on 10,000 patients: Norman J, Goodman A, Politz D. Calcium, parathyroid hormone, and vitamin D in patients with primary hyperparathyroidism: Normograms developed from 10,000 cases. Endocrine Practice. 2011 May-Jun;17(3):384-94
Helpful Videos
- Watch a video of a 4-gland, mini-parathyroid operation that takes less than 13 minutes. This is the parathyroid operation that you want--examine all four parathyroid glands safely and accurately.
- Watch a video of Dr Norman giving overview of Hyperparathyroidism.
- We have an entire page of teaching videos
- Become our patient.
This page was last updated: 01/12/2023




