Different types of parathyroid operations have different cure rates. Operating on one side of the neck (and not looking at all four parathyroid glands) will provide a cure rate of around 80%, BUT, an additional 10% of people who THINK they are cured will need a second surgery within 10 years because they are not cured long-term. See our page on mini-surgery to understand this--the guy we operate on in the video has two parathyroid tumors, and a one-side operation would not have cured him completely or long-term.
The experience of the surgeon has more influence on parathyroid surgery than any other type of surgery. There is nothing more important than finding a surgeon who does parathyroid operations very frequently. Importantly, this does not mean thyroid surgery so don't be fooled by the surgeon that says he "does lots of thyroid and parathyroid surgery". Parathyroid surgery is not like thyroid surgery.
Even the New York Times recognizes that doctors who perform only a few delicate operations per year put patients at undue risk.
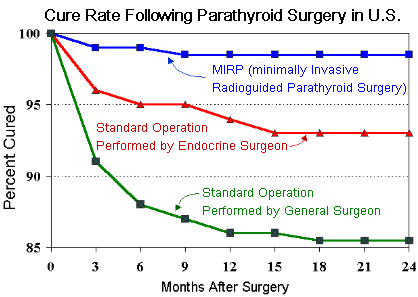 The graph on the right is very important for patients with parathyroid disease to know and understand. There is a big difference in cure rates following parathyroid surgery depending upon which operation is performed, and the amount of parathyroid experience the surgeon has. In fact, there is no other type of surgery that is effected as much by surgeon experience as parathyroid surgery. Some extremely experienced surgeons can perform mini parathyroid surgery on ALL patients. Other surgeons will only perform a mini parathyroid operation if your scan is positive, while the least experienced surgeons (your typical general surgeon or ENT surgeon) will tell you they need to do a big operation and you have to spend the night in the hospital... because "that is the way they do it". You are looking to avoid surgeons who want to look at only one parathyroid gland and measure hormones... this has a cure rate around 85%. When we say "standard operation" we are talking about an operation that looks at all four parathyroid glands. If you do not have all four parathyroid glands examined, then your surgeon is cheating you (read our blog on this topic). Look at this chart and see that the least experienced surgeon will cure you only 85% of the time. See footnotes below for journal citations for these statistics.
The graph on the right is very important for patients with parathyroid disease to know and understand. There is a big difference in cure rates following parathyroid surgery depending upon which operation is performed, and the amount of parathyroid experience the surgeon has. In fact, there is no other type of surgery that is effected as much by surgeon experience as parathyroid surgery. Some extremely experienced surgeons can perform mini parathyroid surgery on ALL patients. Other surgeons will only perform a mini parathyroid operation if your scan is positive, while the least experienced surgeons (your typical general surgeon or ENT surgeon) will tell you they need to do a big operation and you have to spend the night in the hospital... because "that is the way they do it". You are looking to avoid surgeons who want to look at only one parathyroid gland and measure hormones... this has a cure rate around 85%. When we say "standard operation" we are talking about an operation that looks at all four parathyroid glands. If you do not have all four parathyroid glands examined, then your surgeon is cheating you (read our blog on this topic). Look at this chart and see that the least experienced surgeon will cure you only 85% of the time. See footnotes below for journal citations for these statistics.
[Editorial note from Dr Norman... Obviously we can't operate on every parathyroid patient in the US... however nearly 20% of our practice consists of operating on patients that have already had an operation by an inexperienced surgeon--and they were not cured--or worse yet, they were not cured and they can't talk. Yep, from 1 to 3 operations that we do EVERY DAY (out of 12 or 13 that I do every day) have had an unsuccessful parathyroid operation performed somewhere else. I'd prefer that all those inexperienced surgeons would stop doing this operation so we could get at least one experienced parathyroid surgeon in every town... Find the best endocrine surgeon you can!]
- The average number of parathyroid operations that surgeons perform in the U.S. during their residency (surgical training) is only 2 (two parathyroid operations). Data from the American Board of Surgery, 1995 and 2002, footnote at bottom of page.
- The number of parathyroid operations the average general surgeon in practice in the U.S. performs annually is less than 2. This is the same for ENT (ear-nose-throat) surgeons.
- Parathyroid anatomy is the most variable anatomy in the human body.
- The normal parathyroid is the size of a grain of rice, and can be found anywhere in the neck from the jaw down into the chest next to the heart.
- Parathyroid disease can be caused by one bad parathyroid gland, or it can be caused by 2, 3, (or very rarely 4 bad parathyroid glands).
- The complications from parathyroid surgery are serious, and typically WORSE than the disease. Complications are MUCH more common in general surgeons (and ENT surgeons) who do 35 or fewer parathyroid operations per year.
Complications of Parathyroid Surgery.
There are really only two potential complications possible during parathyroid surgery, both of which are not very common but both of which are very serious. However, the type of surgery and the experience of the surgeon affect the potential rate of both complications. The first complication discussed is damage to the nerve to the voice box. The second is the accidental removal of all four parathyroid glands causing the opposite problem of too little (none) parathyroid hormone.
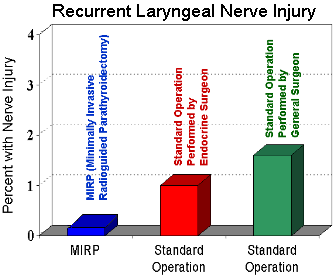 Complication Number One: Injury to the Recurrent Laryngeal Nerve. This graph shows the risk of injury to the nerve that controls the vocal cords. Injury to this nerve during a parathyroid operation can make the patient's voice hoarse. Sometimes the nerve can be stretched or bruised--when this happens the voice is hoarse for a few weeks or even a few months--and then it returns to normal. Sometimes, however, the nerve is cut during the dissection needed to find or remove a parathyroid tumor--in these cases the patients voice will remain hoarse (like a whisper) for a lifetime. There are some procedures that can be done to the vocal cord (like injection of Teflon) to make it work better, but this can be a bad complication.
Complication Number One: Injury to the Recurrent Laryngeal Nerve. This graph shows the risk of injury to the nerve that controls the vocal cords. Injury to this nerve during a parathyroid operation can make the patient's voice hoarse. Sometimes the nerve can be stretched or bruised--when this happens the voice is hoarse for a few weeks or even a few months--and then it returns to normal. Sometimes, however, the nerve is cut during the dissection needed to find or remove a parathyroid tumor--in these cases the patients voice will remain hoarse (like a whisper) for a lifetime. There are some procedures that can be done to the vocal cord (like injection of Teflon) to make it work better, but this can be a bad complication.
The MIRP operation is a much smaller operation, so the risk is the lowest for this operation (less than 1 percent, shown in blue) (less than 1 in 10,000 at our center). The old-fashioned standard parathyroid operation has a nerve injury risk of about 1-2 percent when performed by experienced parathyroid surgeons (shown in red). When performed by surgeons who do parathyroid surgery infrequently, the risk can be as high as 3 or 5 percent (shown in green). NOTE...this may seem like a low rate for this complication, but this is a terrible complication of parathyroid surgery, leaving the patient with a hoarse voice (sometimes forever), and often the patient can't speak except for a whisper. Don't take this lightly! Make sure you discuss this with your surgeon. A parathyroid surgeon who has done over 1000 parathyroid operations will have a risk of this complication of less than 1 in 500... less than 1%, as opposed to a risk of 1 in 25 for a general surgeon who does this operation less than 5 times per year.
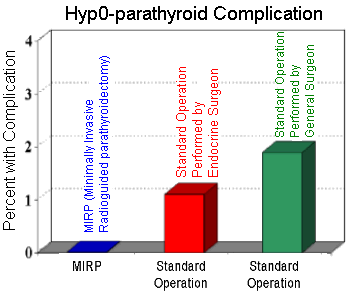 Complication Number Two: Accidental Removal of All Four Parathyroid Glands Causing Permanent Hypoparathyroidism. The second major risk from parathyroid surgery is the removal of all four parathyroid glands (un-intentionally), leaving the patient with NO parathyroid glands. This is called hypOparathyroidism (too little parathyroid hormone) and it can cause some bad symptoms (We have two complete pages on this complication, click here to read more). This complication is also quite rare, but differs according to surgery type and surgeon experience. The MIRP mini parathyroid surgery has a near-zero theoretical risk of removing all four parathyroid glands since glands that are not radioactive do not get removed. The probe prevents the surgeon from removing normal glands! As shown in green, surgeons who do not perform parathyroid surgery very often have a risk of causing hypOparathyroidism nearly double that of experienced endocrine surgeons (shown in red) who have far less than a 1 percent chance of this complication. Again, please note that this is a TERRIBLE complication and will consume your life... please be careful and discuss this with your surgeon. Ask them if it has ever happened to one of their patients and what they will do to assure you that this will not happen to you. Also, realize that your surgeons tells you that "you have 4 bad glands and we have to take out 3.5 glands"...then they are 1) almost guaranteed to be wrong, 2) inexperienced, and 3) much more likely to cause you hyp0parathyroidism. This statement should be a big red flag to you and you must be careful. If a surgeon says this to you based upon a sestamibi scan, you MUST find a different surgeon.
Complication Number Two: Accidental Removal of All Four Parathyroid Glands Causing Permanent Hypoparathyroidism. The second major risk from parathyroid surgery is the removal of all four parathyroid glands (un-intentionally), leaving the patient with NO parathyroid glands. This is called hypOparathyroidism (too little parathyroid hormone) and it can cause some bad symptoms (We have two complete pages on this complication, click here to read more). This complication is also quite rare, but differs according to surgery type and surgeon experience. The MIRP mini parathyroid surgery has a near-zero theoretical risk of removing all four parathyroid glands since glands that are not radioactive do not get removed. The probe prevents the surgeon from removing normal glands! As shown in green, surgeons who do not perform parathyroid surgery very often have a risk of causing hypOparathyroidism nearly double that of experienced endocrine surgeons (shown in red) who have far less than a 1 percent chance of this complication. Again, please note that this is a TERRIBLE complication and will consume your life... please be careful and discuss this with your surgeon. Ask them if it has ever happened to one of their patients and what they will do to assure you that this will not happen to you. Also, realize that your surgeons tells you that "you have 4 bad glands and we have to take out 3.5 glands"...then they are 1) almost guaranteed to be wrong, 2) inexperienced, and 3) much more likely to cause you hyp0parathyroidism. This statement should be a big red flag to you and you must be careful. If a surgeon says this to you based upon a sestamibi scan, you MUST find a different surgeon.
Read more about surgeon-induced hypoparathyroidism and a large study of these patients that was conducted with the Hypoparathyroidism Association of America... by clicking here.
DEAR DR. NORMAN,
Hi! and Help! My name is Mary Jo and I have been diagnosed with hyp0parathyroidism after my surgeon removed all my parathyroid glands when he was trying to find the one bad one. I have been so sick, MUCH worse than I was before the operation. They can't get my calcium to stay in normal ranges. I have been as low as 6.5 and as high as 18.1. When it is low, I feel worse than I ever have in my life. Is there a test to find out if I have any parathyroid glands left? It has been nine months since the surgery. Is it too late to do any thing about it? Can I get a transplant? And what will be my life span if I continue staying like this? Please any suggestions will be very helpful... I am desperate!
Dear Mary Jo,
Regrettably, I get an email just like yours every week. Once you have hyp0parathyroidism, there is very little that can be done... you are simply forced to take huge amounts of calcium and vitamin D every day, and without the parathyroid glands regulating things, your calcium levels will fluctuate from high to very low, and your body simply does not like that. That is the reason you feel so bad. The only hope for patients like you is to take PTH injections every day. This is a very new treatment, but it requires you to inject parathyroid hormone (PTH) into your skin every day just like a diabetic injects insulin into their skin every day. Most people who do the daily injections will have much better control of the calcium fluctuations, and therefore feel significantly better. This is NOT an FDA approved application of this drug, but it may be the only thing that makes you feel better I wish you well!
James Norman, MD, FACS, FACE.
Unsuccessful Parathyroid Operations.
Beside the two main potential complications of parathyroid surgery, there is one other potential problem following parathyroid surgery: Not fixing the problem. As discussed on other pages of this Web site, the anatomy of the parathyroid glands is extremely variable. The four parathyroid glands can be located all over the neck--its the most variable anatomy in the entire human body! Thus, it is possible for a surgeon to operate on you for several hours and NOT find the bad parathyroid gland. Again, the chance of this happening is EXTREMELY dependent upon the experience of the surgeon. Those that do this operation only a few times per year have a probability of not finding the offending parathyroid gland between 5 and 15 percent of the time. These patients are then often referred to the experts so they can re-do the operation. Radioguided techniques (like used in the MIRP operation) has proven to be the best way to find these hidden parathyroid tumors. However, do we need to say??... you would be better of going to an expert parathyroid surgeon for the FIRST operation!
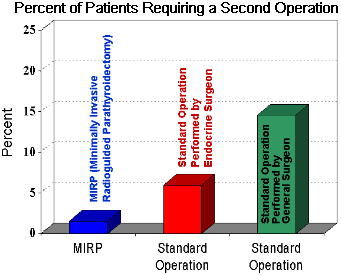 About 18% of our practice is made up of patients that have already been operated on by a general surgeon (or an ENT surgeon) who did not find the bad parathyroid gland. Several clinical studies have shown that radioguided parathyroid surgery is extremely useful in these cases. Once again, the graph on the left shows how the MIRP mini-parathyroid operation has about a one percent chance of not finding the bad parathyroid gland. The standard operation is not near as good, when performed by an endocrine surgeon (shown in red) or by a general surgeon (shown in green). (Editorial note: we do about 400 re-do parathyroid operations per year at the Norman Parathyroid Center... we wish we did not!!).
About 18% of our practice is made up of patients that have already been operated on by a general surgeon (or an ENT surgeon) who did not find the bad parathyroid gland. Several clinical studies have shown that radioguided parathyroid surgery is extremely useful in these cases. Once again, the graph on the left shows how the MIRP mini-parathyroid operation has about a one percent chance of not finding the bad parathyroid gland. The standard operation is not near as good, when performed by an endocrine surgeon (shown in red) or by a general surgeon (shown in green). (Editorial note: we do about 400 re-do parathyroid operations per year at the Norman Parathyroid Center... we wish we did not!!).
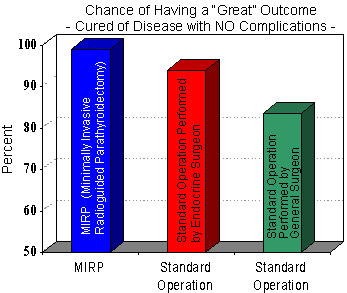 Finally, this graph combines all of the other data into one graph to show the chance of having a 'great' outcome (cured of the disease without any complications from the surgery). You can easily see that an experienced endocrine surgeon performing a MIRP mini-operation (shown in blue) has by far the highest chance of a 'great' outcome. A standard parathyroid operation on both sides of the neck performed by an experienced endocrine surgeon (shown in red) should have a 'great' outcome about 94% of the time, while a standard parathyroid operation performed by a general surgeon (or ENT surgeon) has the lowest chance of a 'great' outcome.
Finally, this graph combines all of the other data into one graph to show the chance of having a 'great' outcome (cured of the disease without any complications from the surgery). You can easily see that an experienced endocrine surgeon performing a MIRP mini-operation (shown in blue) has by far the highest chance of a 'great' outcome. A standard parathyroid operation on both sides of the neck performed by an experienced endocrine surgeon (shown in red) should have a 'great' outcome about 94% of the time, while a standard parathyroid operation performed by a general surgeon (or ENT surgeon) has the lowest chance of a 'great' outcome.
What Qualifies as an "Expert Parathyroid Surgeon" ?
A study from New York University has examined this question by looking at complication rates and cure rates for surgeons of different experience levels and their answer is:
- A surgeon who has performed less than 350 parathyroid operations (in their lifetime) is 'inexperienced'.
- A surgeon who has performed between 350 and 1000 thyroid and parathyroid operations is 'experienced'.
- A surgeon who has performed more than 1000 thyroid and parathyroid operations is called an expert.
Our studies show that surgeons that perform less than 50 of these operations per year have a complication rate nearly 20 times higher than those that do more than 250 per year.
Read what the New York Times says about surgeons who do an operation only a few times per year...
it puts people at undue risk
Study Finds Many Doctors Performing Surgery Lack Practice
February 10, 2003
By RICHARD PEREZ-PENA
A high proportion of the doctors who do delicate medical procedures - and many of the hospitals where they are performed - have relatively little experience at them, according to figures being released this week. Some consumer advocates say the situation may endanger patients.
Dozens of studies have shown that a patient has a much higher risk of serious injury or death at the hands of a surgeon or hospital that handles a particular procedure infrequently. Patient advocates, including the group that is releasing the new information, the Center for Medical Consumers, say the numbers point to a need for the New York State Department of Health and the hospitals themselves to limit which hospitals and doctors provide certain services.
"It's time for the state to seriously consider applying certificate of need to other surgeries," said Arthur Levin, director of the Center for Medical Consumers. "The volume data tells us that there are doctors and hospitals out there doing some surgeries so rarely that it could put people seriously at risk."
One of the procedures studied was thyroid/parathyroid surgery, where 2/3 of the surgeons who performed these operations performed 3 or fewer operations per year!
- Chen H, Zeiger M, Gordon T, Udelsman R. Parathyriodectomy in Maryland, Effects of an endocrine center. Surgery 1996;120:948-53.
- Sosa JA, Powe NR, Levine MA, et al. Thresholds for surgery and surgical outcomes for patients with primary hyperparathyroidism: A national survey of endocrine surgeons. J Clin Endocrinol Metab 1998:83:2658-65.
- McHenry CR. Patient volumes and complications in thyroid surgery. British J Surgery 2002;89:821-823
- Mittendorf EA, McHenry CR. Complications and sequelae of parathyroidectomy and an analysis of surgeon experience and outcome. Surgical Technology International XII. 2003:152-157.
- Norman J, Politz D. Failed parathyroid surgery: The high personal and financial cost of surgeon inexperience. Manuscript in press, 2007.
- Harness JK, Organ Jr, CH, Thompson NW. Operative experience of US general surgery residents in thyroid and parathyroid disease. Surgery 1995;118:1063-70.
- Sosa JA, Bowman HM, Tielsch JM, et al. The importance of surgeon experience for clinical and economic outcomes from thyroidectomy. Annals of Surgery 1998;3:320-30.
- Norman J. Surgeon induced hypoparathyroidism. Proceeds of the annual meeting of the Hypoparathyroid Association. Washington, DC. 2007.
What to read next
- Watch a movie of a minimally invasive parathyroid operation which takes less than 13 minutes.
- Read more about hypoparathyroidism caused by surgeon inexperience and a study done in conjunction with the Hypoparathyroid Association by clicking here.
- How to become our patient




