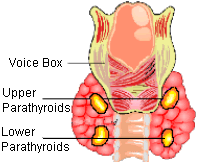
 Parathyroid glands located behind the thyroid. There are 4 parathyroid glands.
Parathyroid glands located behind the thyroid. There are 4 parathyroid glands.
If you have hyperparathyroidism (parathyroid disease), you have about a 70% chance of having one bad parathyroid gland (a benign parathyroid tumor we call a parathyroid adenoma). However, 30% of you will have more than one bad parathyroid gland (two or more). This is why you want your surgeon to examine all four--there is no way to know if a second tumor exists without looking at all four of them.
Since hyperparathyroidism can only be treated with surgery, then it should be obvious to you that the goal of the operation is to remove ALL of the BAD parathyroid glands. It should seem obvious as well, that if you have two bad parathyroid glands and your surgeon removes only one, then you will not be cured. If we can get you to understand this simple fact, then we are half way there! Your parathyroid surgeon must remove all the bad parathyroid glands (and leave the normal ones behind!) or the surgery will be unsuccessful and the patient will not feel better or gain any benefit from the operation. Removing one tumor and leaving a second tumor behind (even a smaller one) does little or nothing for the patient. There is no benefit.
Great Idea!! Let's get a scan or x-ray of some form to tell us how many parathyroid glands are bad, and where these bad parathyroid glands are located! (We wish it were this simple!).
Us surgeons typically want to know what we are operating on before we operate. It makes us more confident before we put a knife on somebody's skin. Similarly, many of you will have an endocrinologist that wants to "see" the parathyroid tumor before he/she sends you to the surgeon. (Editor's note: this is the dumbest thing in the world--it is NOT the job of the endocrinologist to find the parathyroid tumor). Because us doctors like to "see" the tumor before we operate, we have been inventing different scans over the past 30 years in an attempt to "find the tumor". This page is all about that quest, and how dumb it really is--because it can't be done accurately.
Our "Rules of the Scans":
Scans cannot find 50% of parathyroid tumors and when they do, they are wrong 50% of the time.
Sestamibi scans are the best scans to find a parathyroid tumor, BUT, they can find only about 50%. In other words, the tumor is present, but the scan does not have the resolution to find it. Therefore, at least 50% of parathyroid tumors cannot be seen with a sestamibi scan. (did you watch our surgery video showing that the scan was wrong?)
- Sestamibi scans are not as accurate as many doctors will have you believe. When a sestamibi scan is positive, it is wrong about half of the time. In other words, the "parathyroid tumor" they see on the scan is really a thyroid nodule, or the left lower parathyroid is actually the left upper. Don't get excited about your positive scan--it will be wrong half of the time!
- Most sestamibi scans are performed poorly by people who don't do them often, and these scans can't even find 35% of parathyroid tumors.
- Ultrasound can find about 60% of parathyroid adenomas (if the scan is actually performed by an endocrinologist or surgeon, or a tech that is experienced in parathyroid ultrasound and who has been told that that is what they are looking for!). However, ultrasound only finds the easy to locate, superficial tumors. The sound waves do not go deep enough and so they cannot find tumors deep in the neck, those up high in the neck, those in the chest, etc. A parathyroid tumor found on an ultrasound is a parathyroid tumor that any experienced parathyroid surgeon would find during a routine parathyroid operation, with a few rare exceptions.
- Ultrasound performed by a tech at your local x-ray place will find less than 25% of parathyroid tumors primarily because the physician that orders the scan almost always orders a "thyroid ultrasound". Thus the well-meaning, often very talented ultrasound tech doesn't know they are supposed to be looking for a parathyroid gland. We see this every single day and the scan was wasted.
- If scans can't find half of the tumors that exist, then it is obvious that scans cannot be used to determine if a patient has hyperparathyroidism (scans cannot be used as diagnostic tools).
- If scans can't find half of the tumors that exist, then it is obvious that scans cannot be used to determine which patients should have an operation and which patients should be "observed" (scans cannot be used to make management decisions).
- Remember folks, most parathyroid tumors are only the size of an almond or grape and they are supposed to be deep in the neck behind the thyroid. The scans simply can't see the tumors because they are small and are hidden next to all of the other "stuff" in the neck! Also remember that these tumors make you sick because of the hormone they are producing, not because they are "big".
- If scans are so inaccurate at finding parathyroid tumors, then why does your endocrinologist put so much emphasis on it? (This drives us crazy!). If they are so inaccurate, why does your surgeon think he can do a mini-operation simply because he sees it on the scan? What about the other 3 glands? What about the 50% of the time that the scan is wrong? Read our blog on this topic.
- Now you understand why this website says several things over and over: 1) Stop worrying about the scan, 2) stop getting scans, 3) you care about your surgeon's skills, not the scan, 4) CT scans are typically worse than sestamibi and ultrasound and is very over-used. If CT-scans gave reliable results, we would use them, yet we haven't obtained a CT scan in 20 years for people who have not had a parathyroid operation yet. We very strongly believe that the only role for a 4-D CT-scan is in patients who have already had an operation and are not cured. In this very uncommon circumstance we will get a 4-D CT-scan.
- We have several blog articles on this topic. If you read and understand these two blog articles (not very long), you will understand all you need to know about sestamibi scans and why we get them (and why we don't care if the scan is negative). The first is about undescended parathyroid glands up near the jaw, another is about parathyroid tumors in the chest. Read about how positive scans can hurt people because they are often wrong.
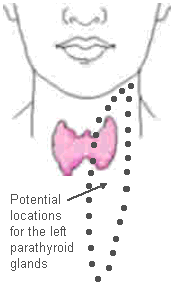 Parathyroid glands have the most unpredictable anatomy in the human body. Parathyroid glands are typically found on the back side of the thyroid gland (para means "around", so parathyroid glands are "around the thyroid glands"). In fact, about 80% of parathyroid glands are found right behind the thyroid gland as shown in the picture at the top-right of this page which is showing the BACK SIDE of the thyroid gland, demonstrating that the four parathyroid glands are closely associated with the back of the thyroid. It really isn't this simple. Because of how parathyroid glands are formed (when we are in our mother's womb), they can be anywhere in the neck from just below the jaw--all the way down into the chest next to the heart. The picture on the left shows the location of the pink thyroid gland in a patient's neck. The black dots outline the possible locations that the left parathyroid glands can be found. You can see that 20% of parathyroid glands are not found next to the thyroid, thus these little guys can be very hard to find! Remember, normal parathyroid glands are only the size of a grain of rice (half of a pea), and get to be about the size of an almond when they develop a tumor (called a parathyroid adenoma) and make too much parathyroid hormone. Knowing this variable anatomy will also help you understand why the experience of the surgeon is so important to a good outcome following parathyroid surgery. Remember, 30% of patients with hyperparathyroidism will have two or more bad glands, and 20% of parathyroid glands are not next to the thyroid, therefore about 40% of people will have at least one parathyroid tumor that is NOT located right behind the thyroid. Since the scans are not good at finding these small guys, you must rely on the experience of the surgeon. If you are reading this page, then somebody will tell you "you must find the most experienced parathyroid surgeon you can".
Parathyroid glands have the most unpredictable anatomy in the human body. Parathyroid glands are typically found on the back side of the thyroid gland (para means "around", so parathyroid glands are "around the thyroid glands"). In fact, about 80% of parathyroid glands are found right behind the thyroid gland as shown in the picture at the top-right of this page which is showing the BACK SIDE of the thyroid gland, demonstrating that the four parathyroid glands are closely associated with the back of the thyroid. It really isn't this simple. Because of how parathyroid glands are formed (when we are in our mother's womb), they can be anywhere in the neck from just below the jaw--all the way down into the chest next to the heart. The picture on the left shows the location of the pink thyroid gland in a patient's neck. The black dots outline the possible locations that the left parathyroid glands can be found. You can see that 20% of parathyroid glands are not found next to the thyroid, thus these little guys can be very hard to find! Remember, normal parathyroid glands are only the size of a grain of rice (half of a pea), and get to be about the size of an almond when they develop a tumor (called a parathyroid adenoma) and make too much parathyroid hormone. Knowing this variable anatomy will also help you understand why the experience of the surgeon is so important to a good outcome following parathyroid surgery. Remember, 30% of patients with hyperparathyroidism will have two or more bad glands, and 20% of parathyroid glands are not next to the thyroid, therefore about 40% of people will have at least one parathyroid tumor that is NOT located right behind the thyroid. Since the scans are not good at finding these small guys, you must rely on the experience of the surgeon. If you are reading this page, then somebody will tell you "you must find the most experienced parathyroid surgeon you can".
One more time for emphasis: There are no scans that can accurately find half of the parathyroid tumors that patients have. The average parathyroid tumor is only the size of an almond, and the scan simply can't find them. Take a look at the pictures of parathyroid tumors and see that about half of them did not show up on a scan! The key to successful parathyroid surgery is not the scan, it's the experience of the surgeon. The key to winning a major golf tournament is not the clubs, it is the guy swinging the clubs.
Tip of the day: Don't keep having tests and more tests, instead find an expert and let him/her take care of it. Don't let your endocrinologist or family doctor keep ordering the scans that are on this page! As much a positive role these doctors play, they really should not be ordering any localizing test. (note, if you come to our center, we will not look at any scans you obtain somewhere else, it will be a waste of time). Let the expert parathyroid surgeon do the scans. As you will read below, most sestamibi scans are done very poorly, therefore, most of you reading this page will get a negative scan and everybody will get confused and all of a sudden things become difficult. Don't get confused, and do not put too much emphasis on these scans. Every single day we get emails from patients who tell us that they have hyperparathyroidism and their doctor sent them for a sestamibi scan and the scan is negative---then everybody goes into a "tizzy" because they don't understand this page. STOP getting all these tests! Find an expert parathyroid surgeon and let them find the tumor.
Many experts feel that no study or test is required to "identify" the diseased parathyroid gland (or glands) prior to an operation for hyperparathyroidism. They feel that surgeons with enough experience can find the problem gland and remove it to cure the disease in about 95% of all cases...without any pre-op tests. Of course what they don't tell you is that this often requires the patient to be under general anesthesia for two to five hours so the surgeon can make a large incision and do an extensive exploration of your neck. What they also don't tell you is that there are only a few surgeons in the US that fall into the "expert" category who can demonstrate a 95% cure rate (most general surgeons have a cure rate between 85 and 90%). The days of making a big incision and exploring the entire neck on all patients with parathyroid disease are gone. The concept is correct, however, and wherever you read about parathyroid disease they will tell you... you want an expert surgeon.
Now that we have told you to stop getting scans we will tell you that every patient should have a sestamibi scan. HOWEVER, the reason to get the scan is not necessarily to find the parathyroid tumor, the scan also shows thyroid nodules, it shows thyroid goiters, it shows "cold" thyroid nodules, it shows the location of the thyroid in the neck, and it shows if there are parathyroid tumors in the chest. We prefer negative scans on our patients. Let me say this again, we prefer that our patients have negative scans, as these are often the easiest operations to perform because the parathyroid tumor is stuck to the back side of the thyroid gland and thus very easy to find! The surgeons at the Norman Parathyroid Center have invented and developed many aspects of modern sestamibi scanning, and we have learned that the NEGATIVE information is much more important than the Positive information. We get scans to show where the tumor is NOT located, rather than showing where it IS located. This change has allowed us to perform a mini operation on 100% of people. Yep, you read that right. We want lots of negative information. A positive scan does not save us 10 seconds in the operating room because we need to find all four parathyroid glands in order to get above 99% cure rates for our patients. Finding the big tumor is easy, its finding the 3 small normal glands that is hard. Please watch our surgery video to understand this more.
Summary of Different Parathyroid Scans
Sestamibi scanning is the best way to find a parathyroid tumor. But as you know, it will only show about half of the parathyroid tumors and is frequently wrong when positive. There are several other tests used that can occasionally discover which parathyroid gland enlarged. Some tests (ultrasound, CAT scan, and MRI scan) simply use pictures of one form or another to find a BIG gland. These studies just look at parathyroid SIZE. Of course, there are other small things in your neck (like lymph glands and thyroid nodules) which can give false tests. Thus, CAT Scans, and MRI Scans should NOT be used to find a bad parathyroid gland. Let us repeat this: If your doctor orders an MRI scan on you to find a parathyroid tumor then get up and walk out. MRI and (and CAT scans to a lesser degree) show less than 5% of ALL parathyroid glands. Therefore, if you have a CAT scan or MRI scan, you have a 95% chance of having a test that costs money, takes time, and won't help a thing (except confuse people).
Ultrasound exams done at your local radiology center or the radiology department of a hospital will also not show the tumor in most cases. Less than 12% of these ultrasound scans will show the tumor... not because the tumor isn't there... but because this test is HIGHLY dependant upon the skill of the person doing the test. If they don't do this every day, the scan will not be useful (like taking a photograph of your kids at night without a flash--you can't see the kids, but the are still there). Ultrasound scans done by endocrinologist or your endocrine surgeon in their office can be helpful and this is a reasonable thing for you to have. If the endocrinologist is not doing it, you probably don't want it. We would NEVER send a patient for an ultrasound test to be done at the local radiology place. However, we do it ourselves on every patient as soon as they get into the operating room, right before we operate. Note, we are evaluating their THYROID also at this time to make sure they don't have a thyroid problem that we can fix at the same time.
When people have a scan to find their bad parathyroid gland and it doesn't show anything, they get confused and their doctor gets confuesed. If the right techniques are not used during your x-ray, it's like taking a picture of the planet Saturn with your cell-phone camera. You take the picture but the photo doesn't show the big planet with the rings. It's not because the planet has disappeared, it's because you used the wrong camera, the wrong film, and the wrong lens to photograph the planet. This occurs hundreds of times per day when patients are sent to their local radiology department for some x-ray to help find the bad parathyroid gland. Unfortunately, at least 75% of you reading this will have already undergone some silly test that didn't help. You will know what we are saying is true, but your inexperienced doctor will order test after test...after test. Stop the silliness.
FNA Needle Biopsy of Parathyroid Tumors. Some endocrinologists and/or surgeons will want to prove that what they believe is a parathyroid tumor on a scan is really a parathyroid tumor, so they will biopsy this gland with a needle. This is called a FNA or "fine needle aspiration" biopsy, or "needle biopsy" of the parathyroid gland. FNA biopsies are frequently done for thyroid nodules, which is appropriate. But FNA for parathyroids is dangerous and should almost never be done. Read a report of this in our blog! A needle needle biopsy of the parathyroid can cause tremendous inflammation around the gland, which leads to scarring, making the parathyroid "stick" to everything around it, possible including the nerve that controls your vocal cords. This makes the operation significantly more difficult for the surgeon, and increases the risks of the operation. Furthermore, the scarring that occurs will look like cancer under the microscope resulting in the pathologist determining that your parathyroid tumor was a cancer... even when it was not. For these reasons, we strongly discourage the use of FNA biopsy for parathyroids. To read our recent publication on this topic in one of the major Endocrinology journals, click here: Diagnostic Aspiration of Parathyroid Adenomas Causes Severe Fibrosis Complicating Surgery and Final Histologic Diagnosis. Thyroid. 2007 Sep 22
The following list describes briefly the different tests which may help a surgeon or endocrinologist find the diseased parathyroid gland which is over secreting parathyroid hormone.
![]() The Sestamibi Scan is now the preferred method for identifying a diseased parathyroid gland prior to an operation. Almost 80 percent correct when it shows a single gland when done by experts that do LOTS of these scans. But 40-50% will be negative regardless of who does it. Therefore, you must understand that this is just a scan and nothing more. Far too much emphasis is put on this scan and the results of this scan. There are technique differences which make these scans at some hospitals much better than they are at other hospitals. Bottom line, it's just a scan. It is way over used. It is emphasized way too much. We wish nobody ever got these scans because they usually confuse people and cause lengthy delays in treatment. If you have a parathyroid problem, you need an expert surgeon not a scan.
The Sestamibi Scan is now the preferred method for identifying a diseased parathyroid gland prior to an operation. Almost 80 percent correct when it shows a single gland when done by experts that do LOTS of these scans. But 40-50% will be negative regardless of who does it. Therefore, you must understand that this is just a scan and nothing more. Far too much emphasis is put on this scan and the results of this scan. There are technique differences which make these scans at some hospitals much better than they are at other hospitals. Bottom line, it's just a scan. It is way over used. It is emphasized way too much. We wish nobody ever got these scans because they usually confuse people and cause lengthy delays in treatment. If you have a parathyroid problem, you need an expert surgeon not a scan.
See our video of The Importance of the Sestamibi Scan.
See our video on How to Interpret Your Sestamibi Scan.
SPECT scanning is a mechanism by which a three dimensional picture can be obtained following injection of the Sestamibi drug. SPECT scanning DECREASES the reliability and accuracy of sestamibi scans, but is done because the radiologist gets paid more to do this. You should refuse this scan. We review over 4,000 sestamibi scans per year, and about 40% of them include SPECT scanning. It is almost never helpful and should not be done. We NEVER use SPECT scanning unless the tumor is in the chest next to the heart. In our opinion, this is the only time SPECT scanning should be used. We cannot stress enough that if you get a SPECT scan, your scan will be LESS valuable and you have at least a 60% chance of the scan being negative, and at least a 70% chance of them "seeing" something on your scan that isn't really there. If you get a SPECT scan somewhere else and then decide to come to our center for your operation, we will not look at your SPECT scan. It provides zero information that will be useful to us.
MRI scans are almost never useful because MRI scans don't show parathyroid tumors well. At best, an MRI will find less than 8% of parathyroid tumors, therefore, the indications for getting this scan are VERY few. We operate on at least on person per week that had an unsuccessful operation somewhere else because the surgeon thought he knew where the parathyroid tumor was--and he saw it on an MRI scan. If your doctor orders an MRI scan to find your parathyroid tumor, stand up, laugh at them, and walk out! IT IS INAPPROPRIATE TO GET AN MRI SCAN ON ANY PATIENT TO TRY TO FIND A PARATHYROID TUMOR. Insurance companies should not pay for it. I hope we made this clear.
CT scans are used much less frequently since the introduction of the Sestamibi scans. They can occasionally be helpful, but getting a CT scan prior to a first operation for hyperparathyroidism is NEVER warranted. THIS TEST SHOULD NOT BE DONE! It does not show parathyroid tumors. Sometimes a patient will have a failed operation and so the doctors start ordering lots of x-rays, including CAT scans. Of course, if you had an experienced surgeon, you are very unlikely to have a failed operation. Thus, get an expert surgeon and don't worry about wasting your time on these dumb tests.
Ultrasound is less costly than CAT scans and MRIs, they are easily performed, carries no significant risks, and can be useful in localizing a parathyroid adenoma. We use ultrasound on all our patients when they are taken to the operating room just before their operation. Only about 12-15 percent of ultrasound scans are correct if they are performed at the local radiology center--therefore, don't waste your time on this scan unless it is performed by your endocrinologist or your surgeon in his/her office. Ultrasound is very accurate when used to examine the thyroid but not for parathyroids--unless done by your doctor! If your doctor just orders this test to be done by some technician at the local hospital or radiology center, then you are wasting your time and money. This is one of the reasons the cost of medicine is going out of control...doctors ordering too many tests even when the tests have little chance of helping.
SESTAMIBI SCANS RESULTS... WHAT TO DO ABOUT YOUR NEGATIVE SESTAMIBI SCAN.
We get to review about 4,500 sestamibi scans per year. These come to us from many hospitals across the US. Sestamibi scans are extremely variable depending on the techniques used. These are NOT regular x-rays which every hospital can perform. Sestamibi scans require the highest degree of technician input. The use of special filters, patient placement, etc, are very important. Therefore, MOST scans done in the US are not very good. About 30% of the scans in the US are WORTHLESS, another 30% are terrible or poor quality.
Sestamibi scanning is often not done correctly, and done for the wrong reasons, and interpreted wrong. Be careful of your sestamibi scan. It can be extremely helpful if your sestamibi scan is positive, but if your scan is negative it doesn't mean much. It does NOT mean you don't have parathyroid disease if your scan is negative (we will say this 10 times so you understand it).
If you have a scan that is "negative" it does NOT mean that you don't have parathyroid disease. It's not negative because you don't have a parathyroid tumor, usually its negative because they do not know how to do this test and a test done poorly won't show the tumor. Or, the parathyroid tumor is simply behind the thyroid gland and so it doesn't show up. Worse yet, your doctor may become confused and tell you to do nothing about your disease--all because some technicians don't know what they are doing! NOTHING ON THIS WEB SITE IS MORE IMPORTANT THAN THIS SIMPLE PARAGRAPH! DO NOT MAKE THIS MISTAKE!
If there was one thing that you should take away from this page it is this... sestamibi scans are very nice tools to help the surgeon know what they are going to find when they open you up. They will know the size of your thyroid, the presence of any thyroid nodules, if your parathyroid tumor is in your chest... but an expert parathyroid surgeon does not care if the scan is positive or negative!
The results of the scan should never be used to determine who goes to surgery and who does not. Using the scan to make this decision is not correct. Almost 75% of the patients we operate on and remove a parathyroid tumor came to see us with a negative sestamibi scan done somewhere else prior to coming to see us. We do the exact same operation on all people, regardless of scan results. Negative scan patients get the exact same operation that takes exactly the same amount of time (17.5 minutes on average), and has the same expected cure rate (over 99%).
This page was last updated: 11/07/2021
What to read next
- Read our blog. It has some really cool patient stories.
- See our map of where our patients come from. COOL!
- Watch Dr Norman examine all four parathyroid glands in 13 minutes.
- How to become our patient




